Save 30-60% on natural products
Noonan Syndrome
Blog post description.
2/4/20266 min read
Please be aware that I post mainly about cancer and Childhood diseases. These are my areas of interest, and while I could grow this substack much faster, it would never have the same personal feel. The sensational news that grows substacks has no appeal for me. I am not the National Enquirer of the Substack community, where fluff and popcorn meet to sell “Sensational and unemotional feel-good pieces.” I may be the Toyota of Substack, but I will still be here while the Cadillacs have run out of gas.
What is Noonan syndrome?
Noonan syndrome is a genetic condition that can affect your child in many ways. While some children born with this condition have mild symptoms, others can have more issues.
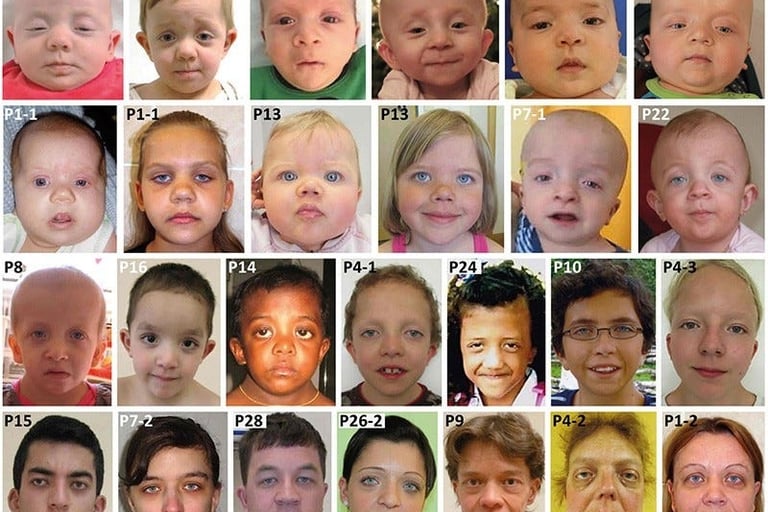
Symptoms typically include unusual facial features such as a tall forehead and wide-set eyes, lower-set ears, and a shorter neck. Many children born with Noonan syndrome also have short stature (short height compared to those of the same age), eye issues, low muscle tone, and congenital (from birth) heart disease.
While Noonan syndrome has no cure, your healthcare provider can recommend guidance to keep your child as healthy as possible. Your provider will also work closely with you to help prevent complications or catch them early, so your child can lead a full, active life.
Who gets Noonan syndrome?
Anyone can be born with Noonan syndrome. About 50% of people with Noonan syndrome have a parent with the condition. In most cases, a person with Noonan syndrome has a 50% chance of passing the condition on to their child.
How common is Noonan syndrome?
Noonan syndrome is a relatively common genetic disorder. It occurs in up to 1 out of every 1,000 to 2,500 people.
Symptoms and Causes
What causes Noonan syndrome?
Noonan syndrome occurs most often due to changes (mutations) in certain genes that help your body’s tissues grow and develop. These mutated genes produce proteins that are active longer than they should be. They interfere with proper cell growth and division.
Noonan syndrome may be:
Inherited:
One parent passes the condition to a child.
Spontaneous mutation:
develops without any family history.
Genetic testing can find an abnormality in almost 80% of people with Noonan syndrome. For the rest, researchers don’t know the exact cause.
What conditions may be similar to Noonan syndrome?
Noonan syndrome belongs to a group of related conditions known as RASopathies (raz-OHP-uh-thees). All of the conditions are due to the same type of abnormal cell growth and development and have similar symptoms.
RASopathies include:
Cardiofaciocutaneous syndrome.
Cardiofaciocutaneous syndrome is a disorder that affects many parts of the body, particularly the heart (cardio-), facial features (facio-), and the skin and hair (cutaneous). People with this condition also have delayed development and intellectual disability, usually ranging from moderate to severe.
Costello syndrome.
Costello syndrome is a rare disorder that affects many parts of the body. This condition is characterized by delayed development, loose folds of skin (which are especially noticeable on the hands and feet), unusually flexible joints, heart problems, short stature, and distinctive facial features.
Neurofibromatosis type 1 (NF1).
Neurofibromatosis type 1 (NF1) is a genetic condition that causes changes in skin pigment and tumors on nerve tissue. Skin changes include flat, light brown spots and freckles in the armpits and groin. Tumors can grow anywhere in the nervous system, including the brain, spinal cord, and nerves.
Legius syndrome.
Legius syndrome (LEE-jus SIN-drome) can cause brown skin spots, armpit freckles, and learning problems. Kids with the condition can manage its symptoms with regular medical care, and have no limits on their activities. It's also known as neurofibromatosis type 1-like syndrome (NF1-like syndrome).
Noonan syndrome with multiple lentigines (formerly, LEOPARD syndrome).
Noonan syndrome with multiple lentigines (NSML) is a condition characterized by lentigines, hypertrophic cardiomyopathy, short stature, pectus deformity, and dysmorphic facial features, including widely spaced eyes and ptosis. Multiple lentigines present as dispersed flat, black-brown macules, mostly on the face, neck, and upper part of the trunk, with sparing of the mucosa. In general, lentigines do not appear until age four to five years, but then increase to the thousands by puberty.
Turner syndrome.
Turner syndrome, a condition that affects only females, occurs when one of the sex chromosomes (X chromosomes) is missing or partially missing. Turner syndrome can cause a variety of medical and developmental problems, including short height, failure of the ovaries to develop, and heart defects.
What are the symptoms of Noonan syndrome?
Symptoms of Noonan syndrome vary from mild to life-threatening, depending on the affected part of your child’s body. Most symptoms start when the fetus is developing in the uterus or appear in children before age 11.
Facial features of children with Noonan syndrome often become less noticeable as children get older. They may include:
Tall forehead.
A deep groove in the middle of their upper lip.
Drooping eyelid (ptosis).
A flat nose with a wide base and bulbous (bulging) tip.
Low-set ears.
Pale blue or green eye color.
Wide-set, downward-slanting eyes that may cross (strabismus).
Other common physical symptoms are:
Bulging toes or finger pads.
Nails that are abnormally shaped or discolored.
Short neck with low hairline or extra folds of skin (webbing).
Short stature.
Sunken chest (pectus excavatum) or raised sternum (pectus carinatum).
Many children born with Noonan syndrome have heart disorders (congenital heart disease). They may require immediate treatment or develop symptoms later in life. Heart conditions include:
Atrial septal defect.
Hypertrophic cardiomyopathy (thickening of the heart muscle).
Pulmonary artery stenosis.
Noonan syndrome may also cause:
Breathing issues, such as laryngomalacia.
A buildup of fluid in the hands or feet (lymphedema).
Developmental delays.
Excessive bleeding or bruising.
Feeding difficulties (in infants).
Testicles that don’t drop (undescended testicles), which can cause fertility issues if not treated.
A curved spine (scoliosis).
Vision problems or hearing loss.
Birth disorders involving the kidneys.
What other complications are associated with Noonan syndrome?
Many children with Noonan syndrome experience slower-than-usual growth in adolescence, although they may be born at a typical length. About 25% have a learning disability, with only some children having an intellectual disability. Around 10% to 15% of children with Noonan syndrome need special education. Noonan syndrome can also cause developmental delays, behavioral issues or speech disorders.
Some children with Noonan syndrome have an increased chance of an unusual childhood leukemia called juvenile myelomonocytic leukemia (JMML) or other childhood cancers. But the overall risk by age 20 is thought to be around 4%.
Diagnosis and Tests
How is Noonan syndrome diagnosed?
Your healthcare provider may suspect Noonan syndrome after a physical exam and review of your child’s symptoms. Your provider may order genetic tests to confirm a diagnosis and rule out other conditions.
Tests may include:
Complete blood count (CBC).
Chest X-ray.
CT scan.
Echocardiogram.
Electrocardiogram (EKG).
Genetic tests.
Ultrasound.
Management and Treatment
Is there a cure for Noonan syndrome?
Noonan syndrome has no cure. But effective treatments can help you and your child manage symptoms.
What is the treatment for Noonan syndrome?
Your child’s healthcare team develops a treatment plan for Noonan syndrome based on your child’s symptoms and their severity. Your child may receive:
Assistive devices such as eyeglasses or hearing aids.
Behavior or speech therapy.
Educational support for learning disabilities.
Medication to ease problems with your child’s heart, treat bleeding, or improve slowed growth.
Growth hormone therapy.
Supportive therapies, such as compression therapy for lymphedema.
In some cases, your healthcare provider may recommend surgery. Early diagnosis is important for effective treatment and follow-up care.
Who might be on my child’s treatment team for Noonan syndrome?
Your team may include your pediatrician and a:
Vascular medicine specialist (blood vessel expert).
Neurologist (brain, spinal cord, and nerves expert).
Oncologist (cancer specialist).
Ophthalmologist (eye care specialist).
Geneticist (genetics expert).
Cardiologist (heart and blood vessel specialist).
Endocrinologist (hormone specialist).
Nephrologist (kidney specialist).
Dermatologist (skin, hair, and nails specialist).
Your care team will recommend a treatment that’s right for your child. They’ll monitor and adjust medications or therapies based on your child’s condition and any side effects they’re having.
Outlook / Prognosis
What’s the outlook for Noonan syndrome?
Most people who have Noonan syndrome lead healthy, independent lives. Your child’s care team will work with you to manage your child’s symptoms and prevent complications.
Prevention
How can I reduce my child’s risk of developing Noonan syndrome?
Nothing you do can reduce your child’s risk of developing Noonan syndrome. It happens because of a genetic change. If Noonan syndrome runs in your family, you can talk to your healthcare provider about prenatal genetic testing.
Living With
When should I seek care for Noonan syndrome?
When Noonan syndrome causes severe congenital heart disease, your child may require surgery and ongoing monitoring to stay healthy and safe. Your healthcare provider can discuss immediate and long-term treatment options with you.